Ozempic: What is it used for, How does it work, What are the side effects?
What is OZEMPIC used for?
- OZEMPIC contains the active ingredient semaglutide, which is used to lower blood sugar levels in individuals with type 2 diabetes.
- OZEMPIC may be used alone if diet and exercise alone are not effective at controlling blood sugar levels, and metformin cannot be used.
- If the treatment for diabetes does not control your blood sugar levels effectively, OZEMPIC is used in combination with one or more other medications. Oral antidiabetics (such as metformin, sulfonylurea, sodium glucose co-transporter 2 inhibitors) or insulin may be included in this category.
- You should follow any diet or lifestyle advice given to you by your doctor, pharmacist, or nurse while using OZEMPIC.
- The use of OZEMPIC is not recommended for patients suffering from Type 1 diabetes mellitus (formerly known as insulin-dependent diabetes mellitus, or IDDM), or for the treatment of diabetic ketoacidosis.
- Ozempic may also help you lose weight.
How does OZEMPIC work?
This medicine belongs to a class of drugs known as GLP-1 receptor agonists (glucagon-like peptide-1 receptor agonists). OZEMPIC works by assisting the body in producing more insulin when it is experiencing high blood sugar levels.
What are the ingredients in OZEMPIC?
Medicinal ingredients: semaglutide.
Non-medicinal ingredients: disodium phosphate dihydrate, propylene glycol, phenol, and water for injections.
OZEMPIC comes in the following dosage forms:
OZEMPIC is supplied in prefilled pens as a clear, colourless solution for injection.
OZEMPIC is available in a carton of 1 disposable, pre-filled, multi-dose pen delivering doses of 0.25 mg or 0.5 mg, including 6 NovoFine Plus needles. This pack size is intended to be used for dose escalation and maintenance treatment at the 0.5 mg dose. The pen contains 1.5 mL solution.
OR
OZEMPIC is available in a carton of 1 disposable, pre-filled, multi-dose pen delivering only doses of 1 mg, including 4 NovoFine Plus needles. This pack size is intended to be used for maintenance treatment at the 1 mg dose only. The pen contains 3 mL solution.
Do not use OZEMPIC if:
- If you are allergic to this medicine or any of its other ingredients, you need not take it.
- You or a member of your family has ever had medullary thyroid cancer (MTC).
- You have Multiple Endocrine Neoplasia syndrome type 2 (MEN 2).
- You are pregnant or breastfeeding.
Before taking OZEMPIC, discuss any health conditions or problems you may have with your healthcare professional. This includes:
- or a member of your family has or has had medullary thyroid carcinoma (MTC), or if you have Multiple Endocrine Neoplasia syndrome type 2 (MEN 2).
- Type 1 diabetes.
- Have ever experienced diabetic ketoacidosis (high blood or urine ketones).
- Known to have an allergy to OZEMPIC.
- A fast pulse (high heart rate).
- Experienced pancreatitis in the past.
- Plan to breastfeed or are breastfeeding.
- Pregnant or planning to become pregnant.
- End-stage renal disease.
- You are suffering from gastrointestinal (digestive) problems, including severe vomiting, diarrhea, and dehydration.
- Hepatic (liver) disease.
- Diabetic retinopathy.
You should also be aware of the following warnings:
Can Children and adolescents use OZEMPIC?
It is not recommended to use OZEMPIC in children and adolescents under 18 years of age since safety and efficacy in this age group has not yet been established.
Driving and using machines:
Low blood sugar (hypoglycemia) may affect your ability to concentrate. Avoid driving or using machines if you get any signs of low blood sugar. See “What are possible side effects from using OZEMPIC” for the warning signs of low blood sugar. Talk to your doctor for further information.
Acute pancreatitis can cause severe and persistent stomach pain:
An inflamed pancreas can cause severe and on-going stomach pain. Consult your doctor immediately if you experience severe stomach pain.
Dehydration:
It is possible to experience nausea, vomiting, and diarrhea during treatment with OZEMPIC. In order to prevent dehydration, it is important to drink a lot of fluids during treatment. If you have any concerns or questions, talk to your doctor.
Diabetic eye disease (retinopathy):
Fast improvements in blood sugar control may lead to a temporary worsening of diabetic eye disease. This may require treatment or lead to a loss of vision. You should inform your doctor if you have diabetic eye disease (retinopathy) or if you experience eye problems during treatment with OZEMPIC.
Tell your healthcare professional about all the medicines you take, including any drugs, vitamins, minerals, natural supplements or alternative medicines.
In particular, tell your doctor, pharmacist or nurse if you are using medicines containing any of the following:
- Sulfonylurea
- Insulin
The risk of getting low blood sugar (hypoglycemia) is increased when these drugs are combined with OZEMPIC. The warning signs of low blood sugar are listed in What are possible side effects from using OZEMPIC. In addition to OZEMPIC treatment, your doctor may advise you to lower your regular dose levels of these medications.
Can you use OZEMPIC during Pregnancy and Breastfeeding?
You should not use OZEMPIC during pregnancy or for at least two months prior to a planned pregnancy because it is not known if it may affect your unborn child.
Contraception is recommended if you are at risk of becoming pregnant while taking OZEMPIC.
The presence of OZEMPIC in breast milk has not been established, so this medicine should not be taken by women who are breastfeeding.
How to take OZEMPIC?
Injections of OZEMPIC are given subcutaneously. They should not be injected into a vein or muscle. The best areas for injections are the front of the thighs, the front of the waist (abdomen), or the upper arm.
Educate yourself on how to use the pen before you use it for the first time.
Make sure you follow your doctor’s directions exactly. If you are not sure, ask your doctor, pharmacist, or nurse.
OZEMPIC should be taken on the same day each week if possible. The injection can be given to you at any time during the day, regardless of meals. When using OZEMPIC once a week, write the chosen weekday (e.g. Wednesday) on the carton to help you remember. In addition, you can write the date on the carton after each injection.
When changing your weekly injection of OZEMPIC, make sure it has been at least 2 days since your last injection.
OZEMPIC should not be stopped without consulting your doctor first. If you stop using it, your blood sugar levels may rise.
What is the usual dose of OZEMPIC?
It is recommended that you use OZEMPIC for four weeks at 0.25 mg once a week, and then increase the dose to 0.5 mg. Talk to your doctor before doing so.
If your blood sugar is not well controlled with 0.5 mg, your doctor may increase your dose to 1 mg once a week.
If your blood sugar is not well controlled with a dose of 1 mg, your doctor may increase it to 2 mg once a week.
It is not a good idea to change your dose unless your doctor has instructed you to do so.
What should you do if you overdose on OZEMPIC?
If you take more OZEMPIC than recommended, talk to your doctor right away. You may experience diarrhea, nausea, or vomiting.
Please contact your healthcare professional, hospital emergency department, or regional poison control center immediately if you think you have taken too much OZEMPIC®.
What should you do if you miss a dose of OZEMPIC?
If you forgot to inject a dose and:
- The last time you should have used OZEMPIC was 5 days or less ago. Use it immediately. Then inject your next dose as usual.
- If it has been more than 5 days since you last used OZEMPIC, skip the missed dose and take your next dose as usual.
Making up for missed doses should not be done by taking an additional dose or increasing the dose.
What are the possible side effects from using OZEMPIC?
OZEMPIC may cause side effects that are not listed here. If you experience any side effects that are not listed here, you should contact your healthcare professional immediately.
There may be side effects associated with this medicine, although not everyone experiences them.
Very common: may affect more than 1 in 10 people:
- Feeling sick (nausea) – this usually goes away over time
- Diarrhea – this usually goes away over time
- Low blood sugar (hypoglycemia) when OZEMPIC is used with a sulfonylurea or insulin.
It is possible for low blood sugar to present itself suddenly with warning signs. Cold sweat, pale skin, headache, fast heartbeat, feelings of nausea or extreme hunger, changes in vision, feelings of sleepiness or weakness, feelings of nervousness, anxiety or confusion, difficulty concentrating or shaking are some of the symptoms. Your doctor will tell you how to treat low blood sugar and what to do if you notice these warning signs.
Common: may affect up to 1 in 10 people:
- Being sick (vomiting)
- Low blood sugar (hypoglycemia) when OZEMPIC is used with an oral antidiabetic other than a sulfonylurea
- Indigestion
- Inflammation of the stomach (‘gastritis’) – this may cause stomach pain, nausea, or vomiting.
- Heartburn and reflux – also known as gastroesophageal reflux disease (GERD)
- Pain in the stomach
- Stomach bloating
- Constipation
- Burping
- Gall stones
- Feeling dizzy
- Feeling tired
- Weight loss
- Less appetite
- Gas (flatulence)
- Increase of pancreatic enzymes (such as lipase and amylase)
- Complications of diabetic eye disease (retinopathy)
Uncommon: may affect up to 1 in 100 people:
- Change in the way food or drink tastes
- Fast pulse
- Injection site reactions – such as bruising, pain, irritation, itching and rash
- Allergic reactions like rash, itching or hives
Rare: may affect up to 1 in 1,000 people:
An allergic reaction of extreme severity (anaphylactic reaction, angioedema). If you experience breathing problems, swelling of your face, lips, tongue, or throat, difficulty swallowing, and a fast heartbeat, you should seek immediate medical attention and inform your doctor right away.
What are the serious side effects of OZEMPIC and what to do about them?
Diabetic retinopathy complications – complications of diabetic eye disease/diabetic eye problems: Talk to your healthcare professional
Pancreatitis (severe and ongoing pain in the stomach area which could be a sign of inflamed pancreas) : Stop taking drug and get immediate medical help
Severe hypoglycemia (low blood sugar) symptoms: feeling confused, fits and passing out: Stop taking drug and get immediate medical help√
Severe allergic reaction (anaphylactic reaction, angioedema) symptoms: breathing problems, swelling of face, lips, tongue and/or throat with difficulty swallowing and a fast heartbeat: Stop taking drug and get immediate medical help
If you have a troublesome symptom or side effect that is not listed here or becomes bad enough to interfere with your daily activities, talk to your healthcare professional.
How to store OZEMPIC?
It is important to keep this medicine out of the reach and sight of children.
Before using a pen for the first time:
- Refrigerate (between 2°C and 8°C). Do not freeze. Do not place near cooling equipment.
During use:
- Pen can be stored at a temperature below 30°C for 8 weeks or in a refrigerator (2°C – 8°C). Do not freeze.
Do not use this medicine if the solution is not clear and colourless.
Do not throw away any medicines via wastewater or household waste. Ask your pharmacist how to throw away medicines you no longer use. These measures will help protect the environment.
How to use OZEMPIC pen inection?
How to inject OZEMPIC 0.25 mg or 0.5 mg doses?
You should not use the pen without proper training from your doctor, nurse, or pharmacist.
Check your pen to make sure it contains OZEMPIC 0.25 mg or 0.5 mg doses. This pen contains 2 mg of semaglutide, and you can select doses of 0.25 mg or 0.5 mg. Your pen can be used with NovoFine and NovoTwist disposable needles up to 8 mm in length. The pack includes NovoFine Plus needles.
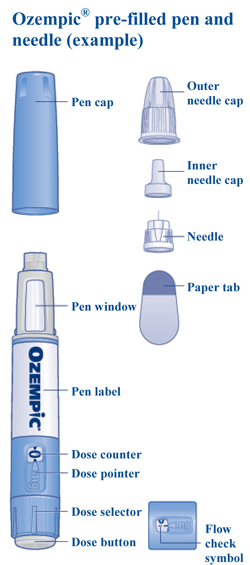
1. Prepare your pen with a new needle
- Make sure your pen contains OZEMPIC 0.25 mg or 0.5 mg doses by checking its name and coloured label. This is especially important if you take more than one injectable medicine.
- Remove the cap from the pen.
- Look through the pen window to ensure that your solution is clear and colourless. Do not use a pen if the solution appears cloudy or coloured.
- Using a new needle, tear off the paper tab. In the event the paper tab is broken, do not use the needle, since sterility cannot be assured.
- Place the needle straight on the pen and turn until it is tight.
- Pull off the outer needle cap and keep it for later. You will need it after the injection, to safely remove the needle from the pen.
- Throw away the inner needle cap. If you try to put it back on, you may accidentally stick yourself.
It is normal for the needle tip to have a drop of solution. Still, you should check that the flow is smooth, if using a new pen for the first time.
You should not attach a new needle to your pen until you are ready to inject. Each injection should be performed with a new needle. By doing this, it prevents blocked needles, contamination, infection, and inaccurate dosing. A bent or damaged needle should never be used.
2. Check the flow
- You should check the flow of your pen before injecting your first injection. If your pen is already in use, go to step 3 ‘Select your dose’.
- You need to turn the dose selector until you see the flow check symbol () on the dose counter.
- Orient the pen so that the needle points up.
Hold the dose button down until the dose counter reaches 0. The 0 must line up with the dose pointer.
You should see a drop of solution at the end of the needle.
It is possible that a small drop will remain at the needle tip, but it won’t be injected. If no drop appears, repeat step 2 ‘Check the flow’ up to 6 times. If there is still no drop, change the needle and repeat step 2 ‘Check the flow’ once more.
In the event a drop is not appearing, dispose of the pen and replace it with a new one.
Before you use a new pen for the first time, make sure a drop appears at the needle tip. This ensures that the solution flows smoothly. If no drop appears, you will not inject any medicine even though the dose counter may move. This may indicate a blocked or damaged needle.
3. Select your dose
- Turn the dose selector until the dose counter shows your dose (0.25 mg or 0.5 mg).
If you select the wrong dose, you can turn the dose selector forwards or backwards to the correct dose.
The pen can dial up to a maximum of 0.5 mg.
How to check how much OZEMPIC is left in the pen?
- To see how much solution is left, use the dose counter: Turn the dose selector until the dose counter stops.
If it shows 0.5, at least 0.5 mg is left in your pen.
If the dose counter stops before 0.5 mg, there is not enough solution left for a full dose of 0.5 mg.
Use a new OZEMPIC pen if your pen does not have enough solution left for a full dose.
4. Inject your dose
- The needle should be inserted into your skin as directed by your doctor or nurse.
- Make sure you can see the dose counter. Do not cover it with your fingers. This could interrupt the injection.
- Hold down the dose button until the dose counter shows 0. This should align with the dose pointer. You should be able to hear or feel a click when the 0 appears.
- Count slowly to 6 after the dose counter returns to 0 and keep the needle in your skin.
- You may see a stream of solution coming from the needle tip if you remove the needle earlier. In this case, the full dose will not be administered if the needle is removed earlier.
- Remove the needle from your skin. If blood appears at the injection site, press lightly. Do not rub the area.
How to identify a blocked or damaged needle while injecting OZEMPIC?
- If 0 does not appear in the dose counter after continuously pressing the dose button, you may have used a blocked or damaged needle.
- In this case, you have not received any medicine even though the dose counter has moved from the original dose that you have set.
How to handle a blocked needle for OZEMPIC injection?
Change the needle as described in step 5 ‘After your injection’ and repeat all steps starting with step 1 ‘Prepare your pen with a new needle’. Make sure you select the full dose you need.
5. After your injection
- Lead the needle tip into the outer needle cap on a flat surface without touching the needle or the outer needle cap.
- Once the needle is covered, carefully push the outer needle cap completely on.
- Unscrew the needle and dispose of it carefully.
- Put the pen cap on your pen after each use to protect the solution from light.
To ensure convenient injections and prevent blocked needles, always dispose of the needle after each injection. If the needle is blocked, you won’t be able to inject any medicine.
When the pen is empty, throw it away without a needle on as instructed by your doctor, nurse, pharmacist or local authorities. It is never a good idea to try to replace the needle cap on the needle. You might get stuck with the needle. After each injection, remove the needle from your pen immediately.
How to care for your OZEMPIC pen?
Treat your pen with care. Rough handling or misuse may cause inaccurate dosing, which may lead to high blood sugar levels or abdominal discomfort such as nausea or vomiting.
- The pen should not be left in a car or any other place where it could get too hot or too cold.
- You should not inject OZEMPIC that has been frozen, as you may develop blood sugar levels that are too high or experience abdominal discomfort, such as nausea or vomiting.
- Do not inject OZEMPIC which has been exposed to direct sunlight. If you do that, your blood sugar level may get too high.
- Do not expose your pen to dust, dirt or liquid.
- Clean your pen with mild detergent on a moistened cloth if necessary. Do not wash, soak, or lubricate your pen.
- The pen should not be dropped or knocked against hard surfaces. If you drop it or suspect that there is a problem, you should attach a new needle and check the flow before injecting.
- Once your pen has run out, it must be disposed of. Do not attempt to refill it.
- Your pen should not be repaired or disassembled.
How to inject OZEMPIC 1 mg doses?
Your pen is a pre-filled dial-a-dose pen. It contains 4 mg of semaglutide, and you can only select doses of 1 mg. Your pen is designed to be used with NovoFine and NovoTwist disposable needles up to a length of 8 mm.
Follow the same instructions as above for injecting 1 mg doses; just select 1 mg when selecting your dose
How to check how much OZEMPIC is left in the pen?
- To see how much solution is left, use the dose counter: Turn the dose selector until the dose counter stops.
If it shows 1, at least 1 mg is left in your pen.
If the dose counter stops before 1 mg, there is not enough solution left for a full dose of 1 mg. - If there is not enough solution left in your pen for a full dose, do not use it. Use a new OZEMPIC pen.
Disclaimer: We have made every effort to ensure that all information is factually correct and up to date, however this article is not comprehensive and does not contain all relevant information about the topic. IT should not be used as a substitute for the knowledge and expertise of a licensed healthcare professional. You should consult your doctor or pharmacist before taking any medication. The drug information contained herein is subject to change and is not intended to cover all possible uses, directions, precautions, warnings, drug interactions, allergic reactions, or adverse effects. The absence of warnings or other information for a given drug does not indicate that the drug or drug combination is safe, effective, or appropriate for all patients or all specific uses.